Spasticity is one of the most frequent neurological complications following stroke. It is characterized by a pathological, velocity-dependent increase in muscle tone associated with upper motor neuron syndrome, often accompanied by hyperreflexia, involuntary muscle contractions, and progressive joint stiffness.
Although classically described as developing weeks after the initial injury, early signs of altered muscle tone can be observed much sooner in clinical practice. Spasticity typically becomes more evident within 4–8 weeks post-stroke and may peak during the first three months. Without timely and appropriate management, it can progressively worsen, leading to significant functional limitations and chronic pain.
Common clinical manifestations include:
- Recurrent involuntary muscle contractions that interfere with voluntary movement
- Progressive joint stiffness, particularly in flexor and antigravity muscle groups
- Pain related to sustained muscle overactivity and abnormal postures
- Reduced ability to perform basic activities of daily living (e.g., dressing, hygiene, feeding)
- Development of fixed contractures due to soft tissue shortening

Beyond its physical manifestations, spasticity substantially impacts overall function and quality of life. It is associated with reduced independence, increased caregiver burden, and higher healthcare utilization. Additionally, it contributes to secondary complications such as pressure ulcers, musculoskeletal deformities, and persistent pain, further limiting rehabilitation potential.
Reported prevalence varies widely (17–80%), reflecting differences in patient populations and assessment methods, but its clinical relevance remains unequivocal.
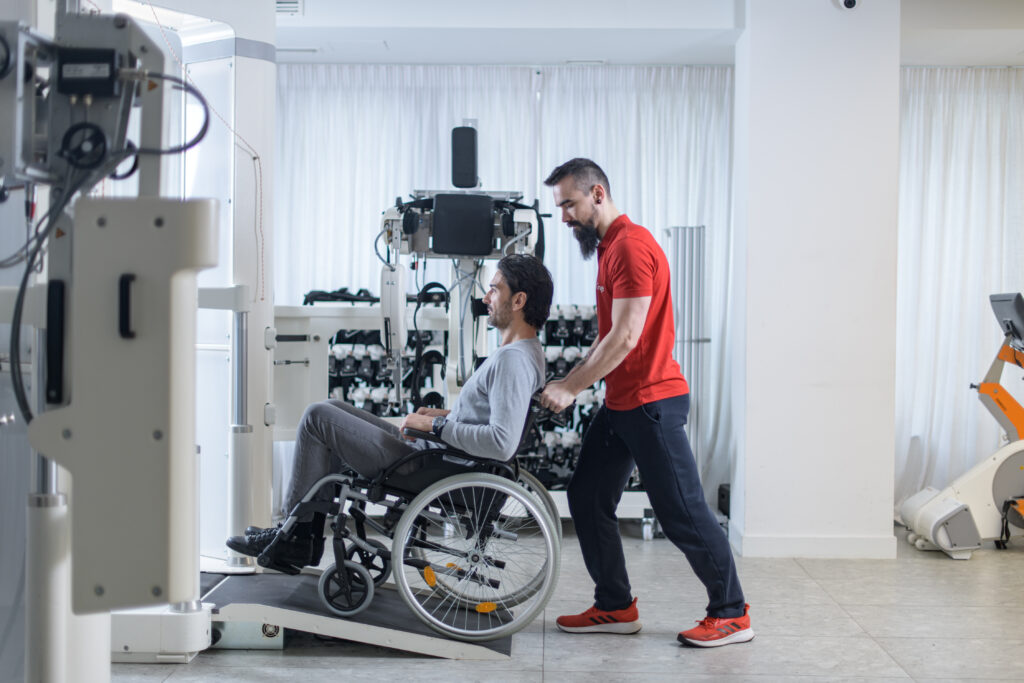
Early therapeutic approach
Current clinical evidence supports early identification and management of patients at risk of developing spasticity, ideally within the first three months following stroke. Risk factors include severe motor impairment, extensive lesions, and involvement of descending motor pathways.
Importantly, early intervention is not limited to reactive treatment but includes preventive strategies aimed at preserving tissue properties, maintaining joint mobility, and promoting more physiological movement patterns.
Effective management requires a structured, multimodal approach combining physical, technological, and pharmacological interventions.
Intensive, robotic-assisted rehabilitation
Repetitive, task-specific training is a key driver of neuroplasticity. In clinical practice, achieving sufficient intensity and movement quality through manual therapy alone can be challenging.
The integration of assistive technologies such as robotic systems, exoskeletons, virtual reality platforms, and focal vibration devices allows for a higher number of precisely guided repetitions, supporting both motor relearning and modulation of abnormal muscle tone. Early active and assisted mobilization has been shown to contribute to improved functional outcomes, particularly in gait and upper limb recovery.

Positioning and postural management
Appropriate positioning of affected limbs in functional alignment helps modulate muscle tone and prevent secondary complications such as pressure ulcers and soft tissue shortening. Consistent postural care also facilitates basic functional activities and improves patient comfort.
Joint mobilization and stretching
Regular passive mobilization and controlled stretching are essential for maintaining joint range of motion and preventing adaptive shortening of muscles and periarticular structures. These interventions support the preservation of soft tissue elasticity and facilitate more selective motor control.
Orthoses and assistive devices
The use of static or dynamic orthoses contributes to maintaining joint alignment, reducing abnormal muscle forces, and preventing deformities. Regular reassessment and adjustment are essential to ensure effectiveness and tolerance.

Post-stroke spasticity represents a significant barrier to functional recovery if not addressed early and appropriately. Its impact extends beyond muscle tone, affecting movement patterns, joint integrity, and overall patient autonomy.
Early, multidisciplinary intervention based on timely assessment, appropriate patient selection, and a coordinated combination of therapeutic strategies is essential to optimize outcomes.
Rather than being viewed solely as a secondary complication, spasticity should be recognized as a dynamic process that can be influenced from the earliest stages of recovery. Delayed or insufficiently intensive management increases the risk of long-term functional limitations that are often difficult to reverse.
In clinical practice, meaningful outcomes are achieved not through isolated interventions, but through a structured and intensive approach that combines precise clinical decision-making with high-repetition, task-specific training. This is particularly relevant in the early stages of recovery, where the potential for neuroplastic change is greatest.


